Connecting rural hospitals in remote areas of the Philippines with mobile mesh networking

While the impact of COVID-19 was felt early on in America’s large cities and urban, metro areas, it became clear that the disease would know no borders and that geographic distance couldn’t slow its spread. But this isn’t a challenge limited only to our country. Around the world, healthcare organizations and governments are fighting simultaneous battles against COVID-19 and the inequities between resources available in modern cities and provisions available in remote, rural areas. This is especially true in the Philippines, where the unique geographic challenges that come with being a nation of thousands of islands are coupled with a lack of modern communications and transportation infrastructure in its more rural areas.
To learn more about the challenges that public health officials are facing in the Philippines, we sat down with Wilfred Alvarez, the Chief IT Consultant at the Philippines Department of Health’s One Hospital Command Center.
During our discussion with Alvarez, we asked about how the lack of communications can impact COVID-19 response, and how mobile mesh networking is being implemented to help coordinate medical and humanitarian aid during the pandemic. Here is what he told us:
The Last Mile (TLM): For our readers that have never been to the Philippines, what are the areas outside of the major urban centers like in terms of terrain, climate and geographical challenges?
Wilfred Alvarez: There are two kinds of weather in the Philippines – summer and the rainy season. We’re currently entering into the summer timeframe right now, which can be very hot because we’re very close to the Equator.

The Philippines is comprised of 7,000 islands, including Mindanao and the big islands, and a number of smaller islands. If you put all of those islands together, they would have the world’s longest shoreline.
On the larger, northern islands there are a number of large, metropolitan areas and cities. Metro areas like Manila are actually comprised of large cities. Manila, itself, consists of thirteen cities. However, outside of those large, urban areas, the rest of the country is mostly rural and agricultural. And, while many people leave these areas to travel to the cities in search of work and jobs, these rural areas remain highly populated.
TLM: How developed are these areas when it comes to critical infrastructure? Communications infrastructure?
Wilfred Alvarez: The metropolitan areas and urban centers have established terrestrial communications infrastructure. For example, the 15-18 million people that live in Manila have access to all of the modern communications solutions and capabilities that you’d expect to find in a modern, major city. However, when you get outside of the urban areas and into the more remote, rural areas where there are smaller, agrarian villages, that communications infrastructure ceases to exist.
“The more remote provinces lack communications infrastructure, but they also have poor transportation infrastructure, as well. In most cases – because they’re islands – the only options are to travel by boat or plane…then, once you arrive, the roads in these areas aren’t even paved.” – Wilfred Alvarez
There are a number of reasons for that. In these less populated areas, the mobile companies and communications companies don’t want to build up their networks because they don’t view it as profitable. There is also some instability in areas of the nation as a result of religious and political differences. This adds to the hesitancy of the communications companies because they don’t want to invest in infrastructure that may be destroyed in a political conflict.
While it would be optimal for rural communities to rely on fiber, sometimes the only choice they have is satellite or point-to-point microwave communications, which is far more expensive.
These factors have led to the rural areas receiving fewer government services and lacking critical traditional communications infrastructure.
TLM: COVID obviously knows no borders and impacts people indiscriminately. How hard have the rural areas of the Philippines been hit by the pandemic?
Wilfred Alvarez: There are 110 million people living in the Philippines. Approximately 60 percent of them are in major cities. But that means approximately 44 million people still live in the more rural, remote provinces.
The more remote provinces lack communications infrastructure, but they also have poor transportation infrastructure, as well. It can be difficult just to get to some of these more remote places. In most cases – because they’re islands – the only options are to travel by boat or plane, which can be very expensive. Then, once you arrive, the roads in these areas aren’t even paved.
This has made keeping track of the COVID-19 pandemic very difficult. With so many people in these hard to reach and hard to communicate with locations, we struggle with a lack of transparency about what’s happening across the country. But, while we may not necessarily know or see it, COVID is making its way to every region and population within the Philippines, including indigenous tribes.
“However, in the rural areas, coordinating [patient transport] and reporting [COVID cases] is a challenge because internet connectivity, cell phones, and landlines are not available outside of major cities.” – Wilfred Alvarez
For example, a new tribe was recently discovered that has been living in the mountains in isolation for quite some time. This tribe was there for generations without exposure to civilization or the outside world. Backpackers interacted with them and brought COVID with them.
So there really aren’t any populations that are safe or immune to the impact of this pandemic. In fact, as of March 2021, we hit our highest number of confirmed COVID-19 cases – around 8,000 newly reported cases. This has caused the government to send in the military to secure places, adding more challenges to an already hard-hit country and economy.
TLM: What unique challenges do first responders and medical personnel face when it comes to their response to COVID in this part of the world?
Wilfred Alvarez: Between public and private hospitals, there are 3,400 total hospitals in the Philippines. Most of those hospitals are “Level One” hospitals that have the least service capability. The hospitals with the highest service capability are in the national capital region, at the northern part of the country near Manila.
It is my job to connect both public and private hospitals and create one hospital command center for the coordination of the COVID-19 pandemic response. As part of the response activities, it is our responsibility to track when positive patients are identified and where they are transported to by emergency medical personnel. Ambulances and paramedics are deployed to them and the most critical patients are transported to the municipal hospital.
“One of the largest challenges that we face is getting the expertise of physicians into the rural areas where the pandemic is spreading so that we can better diagnose and treat patients in those areas. We need to accomplish that by connecting paramedics and emergency medical personnel with the doctors because there’s really no way to safely send doctors into those locations.” – Wilfred Alvarez
However, in the rural areas, coordinating and reporting this is a challenge because internet connectivity, cell phones, and landlines are not available outside of major cities. It costs too much to set up cell sites for emergency connectivity. In the more remote locations, satellite phones are the only option, and they are also very costly to procure and use.
This makes it incredibly difficult to coordinate the activities of paramedics and ambulances, and also makes it difficult to consult medical professionals from the large hospitals in the country’s urban areas should they need help.
TLM: Why is it essential that first responders and emergency medical personnel be able to communicate with COVID patients in isolated and rural areas? What could potentially happen if that communication isn’t there?
Wilfred Alvarez: One of the largest challenges that we face is getting the expertise of physicians into the rural areas where the pandemic is spreading so that we can better diagnose and treat patients in those areas. We need to accomplish that by connecting paramedics and emergency medical personnel with the doctors because there’s really no way to safely send doctors into those locations.

Because of the political instability, the only way that we could send doctors into these regions is with a military or police escort. If an area is currently embroiled in any political turmoil or experiencing any insurgent activity, it’s difficult to risk the lives of doctors by sending them into those areas.
So instead of bringing the physicians to the patients, we need to find a way to connect the paramedics and emergency medical personnel in these remote areas with the doctors back in the large hospitals in the urban, metropolitan areas of the country.
TLM: Why are mobile mesh networks a good solution to this problem? How could mobile mesh be used to connect emergency medical personnel with physicians and hospital staff?
Wilfred Alvarez: In many of these remote locations, the primary form of transportation is also the most reliable form of communication – the motorcycle. People get on motorcycles and the news gets spread around person-to-person. But that’s not an accurate or rapid method of communication. And peer-to-peer, face-to-face communication is not ideal in a pandemic.
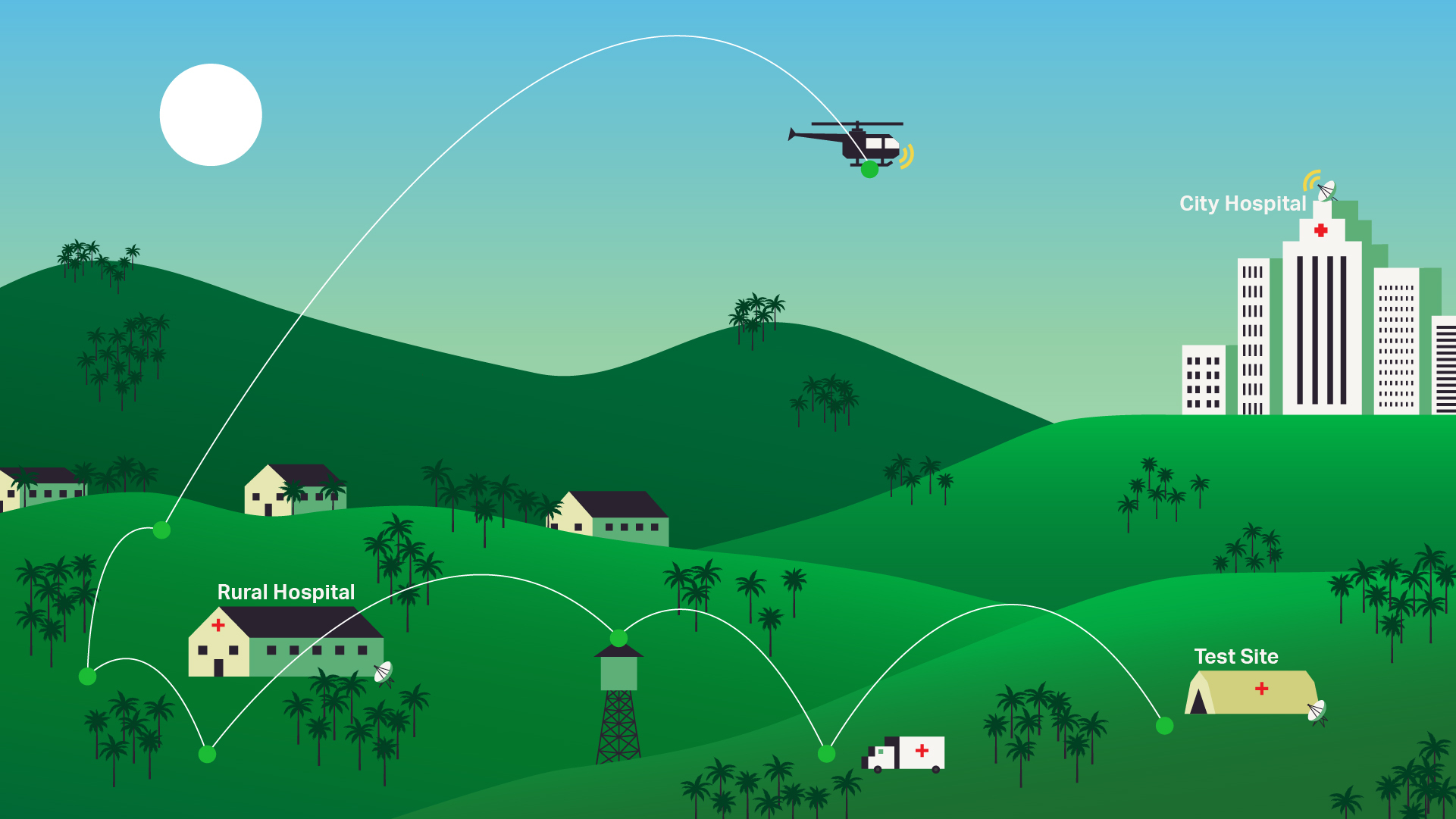
Mobile mesh networking is enabling us to connect these remote areas by relaying information from one node to the next. It enables these government workers to track their team members on a map and allows them to text each other because the bandwidth used is so low and therefore, inexpensive.
In many of the metropolitan areas of the country, unlimited text messaging is available through mobile companies for as little as 50 cents. This has made text messaging a widely-used and relied-upon form of communication. Mobile mesh gives us the ability to use that same form of communication over long distances and in places where the mobile companies don’t have networks.
TLM: Is the connectivity enabled by mobile mesh adequate for this purpose? Why would it be preferred over something with higher bandwidth, like satellite?
Wilfred Alvarez: Satellites are nice, but they’re very expensive. In addition to purchasing the necessary hardware, you have to pay per minute to use the service, and that adds up quickly over time. I – personally – used to have a satellite phone and it was very expensive to pay for the equipment and that per-minute service fee.
With mobile mesh networks, we get a form of communication that we’re all comfortable and familiar with, and we pay no recurring per-minute cost to use that connectivity.
TLM: How far along are you in implementing mobile mesh networking in the Philippines for COVID-19 relief efforts?
Wilfred Alvarez: The mobile mesh networking solution from goTenna Pro has been rolled out to some of our military members. We chose that solution because of its small form-factor and ability to connect to smartphones, which are widely available here in the Philippines.
We’re currently in the process of raising awareness and demonstrating the benefits of connectivity through mobile mesh networking and the goTenna devices. We’ve been demonstrating and presenting the technology to the individual remote regions and provinces. But there is certainly an awareness challenge that we need to overcome.
Soon, we’re looking to start testing it more widely in the more remote, rural areas. However, early usage by local police departments and other government organizations has been very well received and has spurred interest in using this technology.








No Comment